Blog
- All
- 25th May Pre Congress
- 26th May Day 1 Congress
- 28th May Day 3 Congress
- Administrative Councillors
- books
- Chairs
- Clinical Ultrasound
- COE Centre
- COE Task Force
- Collaboration Committee
- Committees
- Congress 2022
- Congress Committee
- Congress News
- Constitution Committee
- E-Book
- E-learning Task Force
- echoes
- Education Committee
- EXB
- Featured
- Featured_Congresses
- Featured_External Meetings
- Featured_Federation
- In Memoriam
- Investment Advisory Committee
- NEWS
- NEWS CoE's
- NEWS Partnerships
- Nominating Committee
- Pioneers
- Publications Committee
- Room 1 - Alfa 1
- Room 1 - Alfa 1
- Room 2 - Alfa 2
- Room 2 - Alfa 2
- Room 3 - Alfa 3
- Room 4 - Atena
- Room 4 - Atena
- Room 5 - Viena
- Room 6 - Roma 1
- Room 7 - Roma 2
- Room 8- Oslo
- Safety Committee
- Safety Statements
- Student Education
- Ultrasound the Best
- UMB Publications
- Uncategorized
- Webinars
- WIOTM
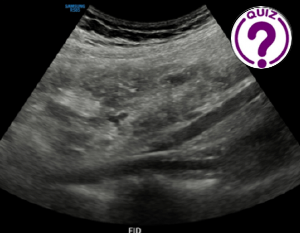
August 22, 2025
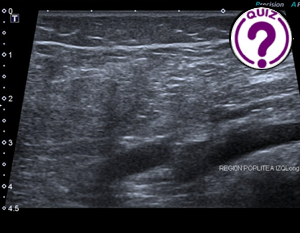
Edda Leonor Chaves S MD * Servicio de Radiología Hospital Nicolas Solano La Chorrera Panamá Correspondence: echavess@minsa.gob.pa Clinical history A 17-year-old female patient is referred from […]
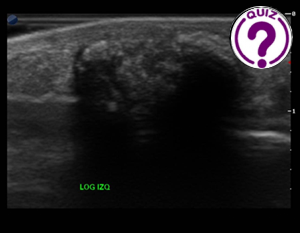
July 1, 2025
JIHENE BELHADJ ALI 1, ASMA KHEZAMI2 ,DOUIRA-KHOMSI WIEM 3 1 Affiliation 1; bhjjihene@gmail.com 2 Affiliation 2; asmakhezami95@gmail.com 3 Affiliation 3; wiem.khomsi@gmail.com Department of Pediatric Radiology, Bechir […]
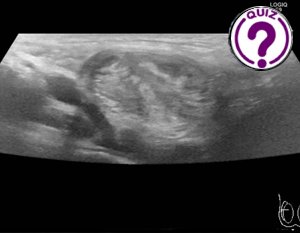
June 3, 2025
1 Raphael Hauser; raphael.hauser@regionh.dk 2 Chenxi Huang; chenxi.huang.01@regionh.dk * Correspondence: raphael.hauser@hotmail.com Clinical history A 50-year-old male with a medical history of congenital chloride diarrhea, intrahepatic biliary […]
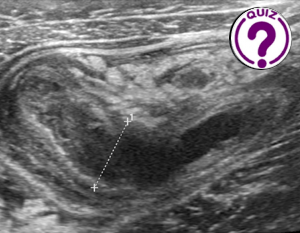
May 1, 2025
Evelina Atanasova 1, Christo Pentchev¹, Dimitar Popov¹ and Christian Nolsøe² 1 Clinic of Gastroenterology, University Hospital „St. Ivan Rilski” Sofia, Bulgaria; e-mail: eva_gatanasova@abv.bg; ch.pentchev@gmail.com, dr_popov@yahoo.com 2 […]
April 1, 2025
Edda Chaves 1* 1 Hospital Regional Nicolas Solano La Chorrera. Panamá *correspondence: echavess@minsa.gob.pa Clinical history A 25-year-old female patient consulted a dermatologist due to the presence […]
March 3, 2025
Alexander Berkfors 1 and Samir Jawad 1 1 Department of Radiology, Rigshospitalet, Copenhagen University Hospital, Denmark * Correspondence: alexander.skovbaek.berkfors@regionh.dk Clinical history An otherwise healthy 7-year-old boy […]
February 3, 2025
Rute Santos 1,2,3* 1 Polytechnic University of Coimbra, Coimbra Health School, Rua da Misericórdia, lagar dos Cortiços, S. Martinho do Bispo, 3045-093 Coimbra, Portugal 2 H&TRC—Health […]
January 13, 2025
Bahareh Abdolalizadeh 1*, Samir Jawad 1 1 Department of Radiology, Rigshospitalet, Copenhagen University Hospital, Copenhagen, Denmark; bahareh.abdolalizadeh.01@regionh.dk * Correspondence: bahareh.abdolalizadeh.01@regionh.dk Clinical history An 11-year-old girl presented […]
December 2, 2024
Edda Chaves 1,* 1 Servicio de Radiología. Hospital Regional Nicolas Solano La Chorrera. Panamá; echavess@minsa.gob.pa * Correspondence: echavess@minsa.gob.pa Clinical history A 45-year-old female was evaluated in […]